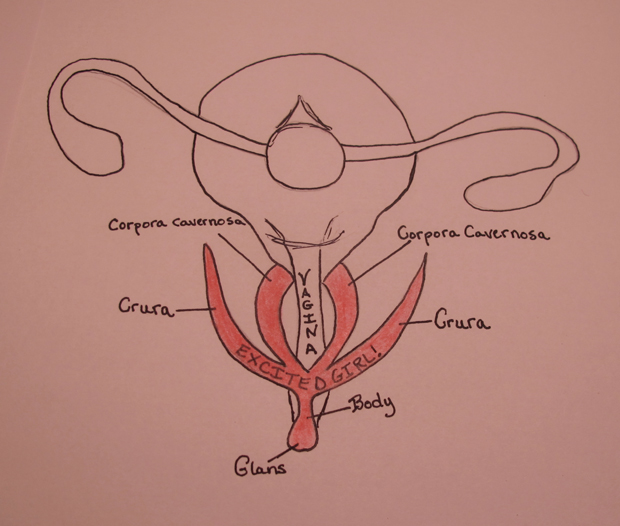
Before I get into PN versus PNE, I want to first give you a brief explanation of the physiology of the pudendal nerve and the diagnosis of PN.
The pudendal nerve is a large nerve that arises from the S2, S3, and S4 nerve roots in the sacrum, and divides into three branches—the inferior rectal nerve, the perineal branch, and the dorsal clitoral/penile branch. The nerve travels a tortuous course through the pelvis to innervate:
• the majority of the pelvic floor muscles,
• the perineum,
• the perianal area,
• the distal third of the urethra
• part of the anal canal
• the skin of the vulva, the clitoris, portions of the labia in women,
• and the penis and scrotum in men.
The pudendal nerve travels a torturous course through the pelvis.
Patients with PN can have tingling, stabbing, and/or shooting pain anywhere in the territory of the nerve. Symptoms include vulvar or penile pain, perineal pain, anal pain, clitoral pain, and pain at the ischial tuberosities as well as pain with bowel movements, urination, and orgasm.